Family Medicine Initiative on Trauma Informed Care (FIT)
We are proud to announce CAFP’s new peer-to-peer learning initiative, Family Medicine Initiative on Trauma-Informed Care (FIT). This is part of CAFP's broader efforts to provide information and education on Adverse Childhood Experiences (ACEs) and Trauma Informed Care. See our website for updated information.
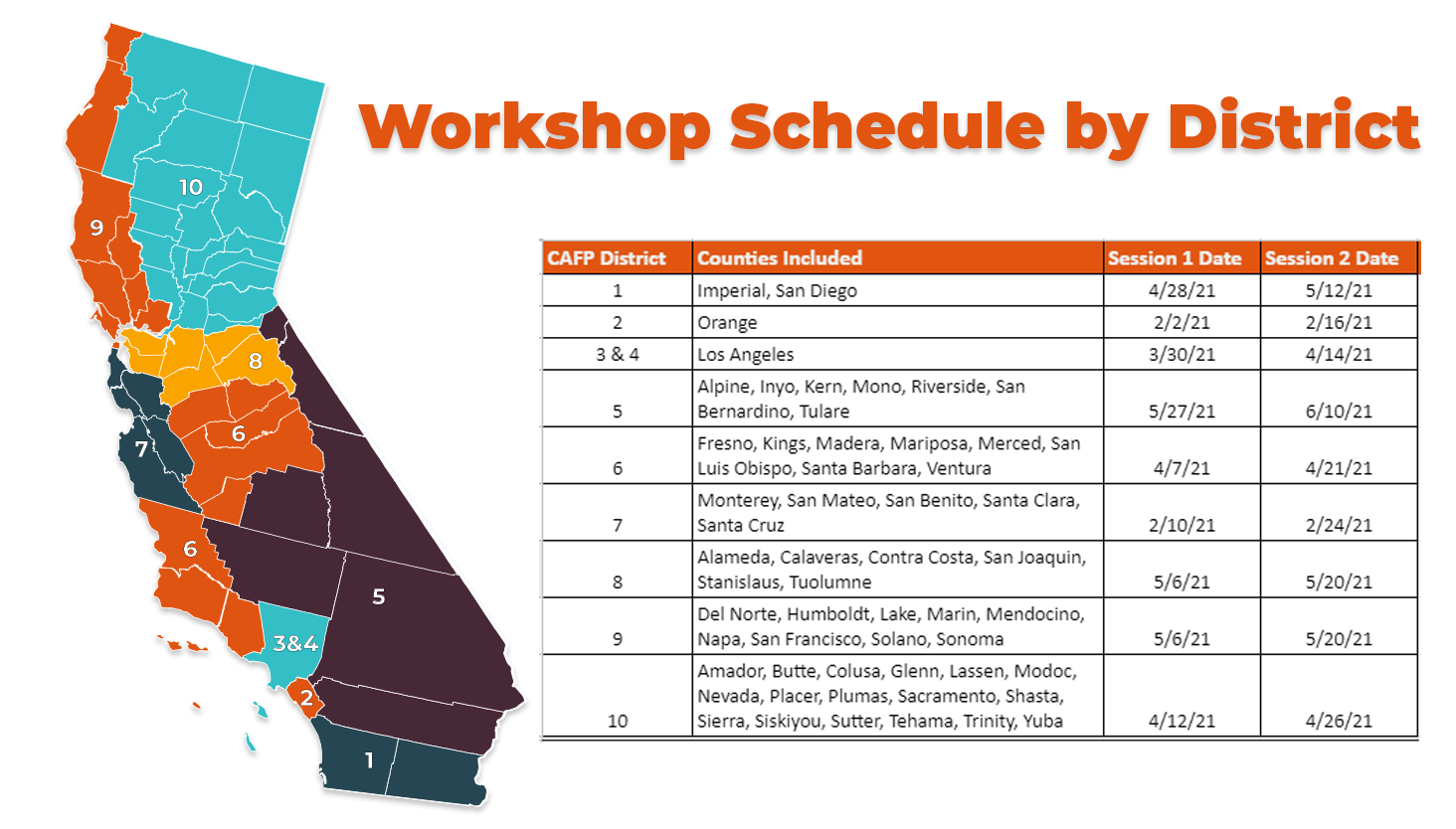
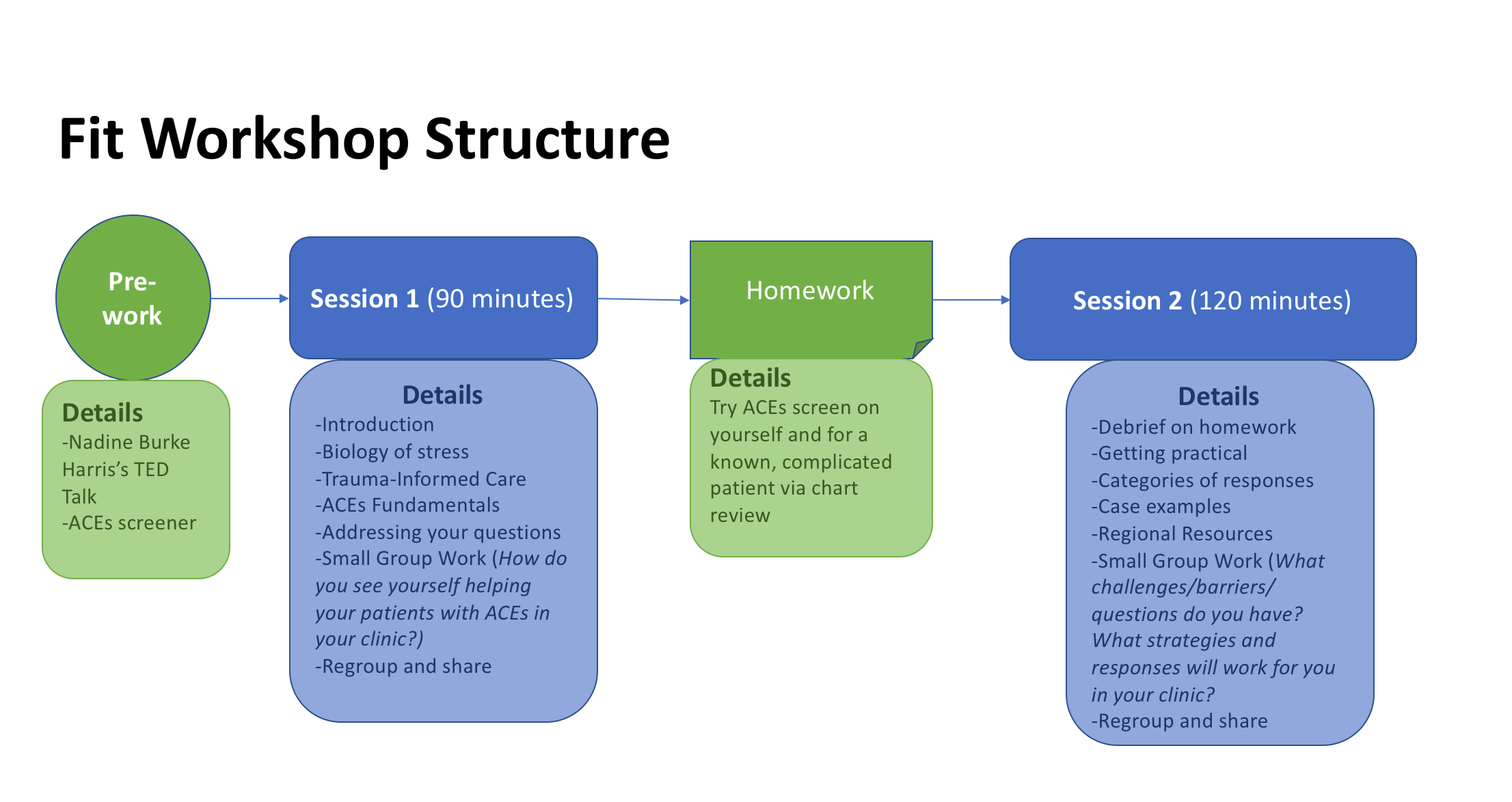
CAFP's Family Medicine Initiative on Trauma-Informed Care (FIT) workshops, each consisting of two sessions, two weeks apart, are designed to introduce clinicians to the concepts of toxic stress and Adverse Childhood Experiences (ACEs) as they relate to trauma-informed care.
It is expected that learners will register for both session 1 and session 2 in their local district. In the first session, participants will learn about the relationship between toxic stress and chronic disease, how to screen for ACEs, and meet in small groups to discuss trauma-informed care. In session 2, the focus will shift to best practices, practical strategies to use when responding to ACEs in their patients, as well as regional/state resources to use with patients. Learners who attend both sessions, and participate in the Translation to Practice (t2p) Commitment to Change process can claim up to 6 AAFP Prescribed CME credits.
Statement of Need:
Adverse Childhood Experiences (ACEs) and toxic stress are public health crises. ACEs are stressful or traumatic events experienced by age 18, identified in the landmark Centers for Disease Control and Prevention (CDC) and Kaiser Permanente (KP) Adverse Childhood Experiences Study, to be strongly associated with increased health and social risks. Early detection and intervention can help prevent or reduce the health risks associated with ACEs.
Support:
This activity is supported by an educational grant from Aurrera Health Group on behalf of the California Department of Health Care Services, and ACES Aware campaign.
Target Audience
The Family Medicine Initiative on Trauma-Informed Care (FIT) workshops are intended for family physicians practicing in the state of California.
Learning Objectives
At the end of this workshop, you should be able to:
- Describe how ACEs and toxic stress disrupt physiology and influence the development of chronic disease
- Summarize the principles of trauma-informed care as they relate to provider, staff and patient wellness
- Formulate practical methods for responding to ACEs with trauma-informed care principles
- Identify best practices in the use of validated ACE screening tools
- Reference regional resources to use with patients
- Provide feedback/suggestions to CAFP for ACEs screening road map
Anna Askari MD, MSBS

Anna Askari is a third year family medicine resident at Eisenhower Health in Rancho Mirage, California. She majored in political science and minored in Spanish at The Ohio State University, received her Master of Science in Biomedical Sciences at the University of Toledo, and graduated with her medical degree from The Ohio State University College of Medicine. She is passionate about integrative/functional medicine as well as underserved medicine. She has served as a medical student and resident leader in the Ohio, California, and AAFP advocating for health care policy to benefit her patients. She is the current resident director on the AAFP Board of Directors, and has accepted a position as an outpatient family medicine physician with One Medical in Aliso Viejo, California once she graduates from residency.
Erika Roshanravan, MD

Erika Roshanravan is a family physician at CommuniCare Health Center, a Federally Qualified Health Center in Woodland, California. She also supervises and teaches University of California, Davis family medicine residents during their continuity clinic at CommuniCare. She received her Doctor of Medicine degree from the University of Berne School of Medicine (Berne, Switzerland) and completed her Family Medicine Residency at University of Washington. She is currently President of CAFP’s Sacramento Valley Chapter Board of Directors as well as Alternate Director for District 10 on the CAFP Board of Directors. Erika is fluent in German, Spanish, French and English and lives with her husband and three children in Davis, California.
Adia Scrubb, MD, MPP

Adia Scrubb is an Oakland native and currently practicing full-scope Family Medicine at LifeLong Medical in East Oakland. She is serving on the California Surgeon General's ACEs Aware Clinical Implementation subcommittee. She received her Doctor of Medicine degree from the David Geffen School of Medicine and PRIME Program at the University of California, Los Angeles (UCLA) and the Charles R. Drew University of Medicine and Science in Los Angeles. She earned a Master of Public Policy degree from UCLA’s Luskin School of Public Affairs and a Bachelor of Arts degree from University of California, Berkeley in Comparative Literature.
Brent Sugimoto, MD, MPH, AAHIVS, FAAFP

Brent K. Sugimoto is a family physician and HIV specialist. With a focus on care for adolescents and adults living with HIV at Kaiser Permanente in Oakland, California he worked to improve outcomes for this population. It was at Kaiser Permanente that Brent began efforts to screen and intervene for Adverse Childhood Experiences, which are over-represented in persons living with HIV. Brent is an educator and author of ACEs education for primary care, he serves on several of the California Surgeon General's ACEs Aware subcommittees, and he is currently the New Physician member on the AAFP Board of Directors. Brent is currently Chief Medical Officer for Decoded Health, a technology startup using artificial intelligence (AI) to achieve the Quadruple Aim. Brent received his MD from the University of California, San Francisco (UCSF), his MS as part of the University of California, Berkeley-UCSF Joint Medical Program, and his MPH from UC Berkeley. Brent lives with his husband and two children in Richmond, California.
Conflict of Interest Statements:
The CAFP Committee on Continuing Professional Development is responsible for management and resolution of conflict for any individual who may have influence on content, who have served as faculty, or who may produce or help produce CME/CPD content for the CAFP. Management/Resolution may include learner notification, peer review of content before presentation, changing topics, or even dismissing a potential faculty member.
It is the policy of the CAFP to ensure independence, balance, objectivity, scientific rigor, and integrity in all continuing education activities. All individuals with potential to influence the content of this program have submitted Conflict of Interest declarations that have been reviewed according to policy. Learner notification of declarations is below. All individuals with potential conflicts have been contacted by CAFP staff or CCPD members, and issues of conflict have been discussed, managed, and resolved.
The FIT expert faculty, planners and staff have no financial relationships with companies that are ineligible to be accredited in the ACCME System to disclose. Ineligible companies are those whose primary business is producing, marketing, selling, re-selling, or distributing healthcare products used by or on patients.
Session 1 is accredited for 1.5 AAFP Prescribed Credits.
Learners who choose to participate in the Translation to Practice/Commitment to Change process can earn an additional 2 AAFP Prescribed Credits.
There are 3.5 AAFP prescribed credits available from Session 1.
--------------
Session 2 is accredited for 2.5 AAFP Prescribed Credits.
--------------
Overall, up to 6 AAFP Prescribed Credits available for participating in the two FIT Initiative sessions.

 Facebook
Facebook X
X LinkedIn
LinkedIn Forward
Forward